In October, the Partners for Rural Transformation (PRT) collaborated with the Urban Institute for an event addressing a national crisis: the health and wellness of our country. The event, Advancing Rural Health Equity through Partnerships, Data, and Finance fostered a discussion around rural American regions and communities experiencing increasingly dismal health outcomes. Over 40 people joined in person, and over 300 people attended virtually. A wide variety of stakeholders attended, including staff from Wells Fargo, several USDA offices, multiple state health departments, USDA Rural Partners Network, numerous universities, U.S. Department of Veterans Affairs, Humana, Housing and Urban Development (HUD), FHFA, land trust organizations, non-profit organizations, CDC, Research Hospitals, Library of Congress, school nurse associations, and White House staff.
The diversity of the attendees directly reflected what is required to generate positive rural health outcomes: strategic multi-sector partnerships advancing rural health equity together. The Partners for Rural Transformation exemplify how regional and national Partnerships are essential to generating positive change in rural communities.
The United States is in an alarming juncture of some of the poorest health outcomes it has seen despite how far we’ve come in health technology. For the first time in modern American history, average life expectancy is declining, despite multi-trillion dollars invested into healthcare systems. The decline started well before the COVID-19 pandemic – experts started noticing declines in life expectancy across the country as early as 2014.
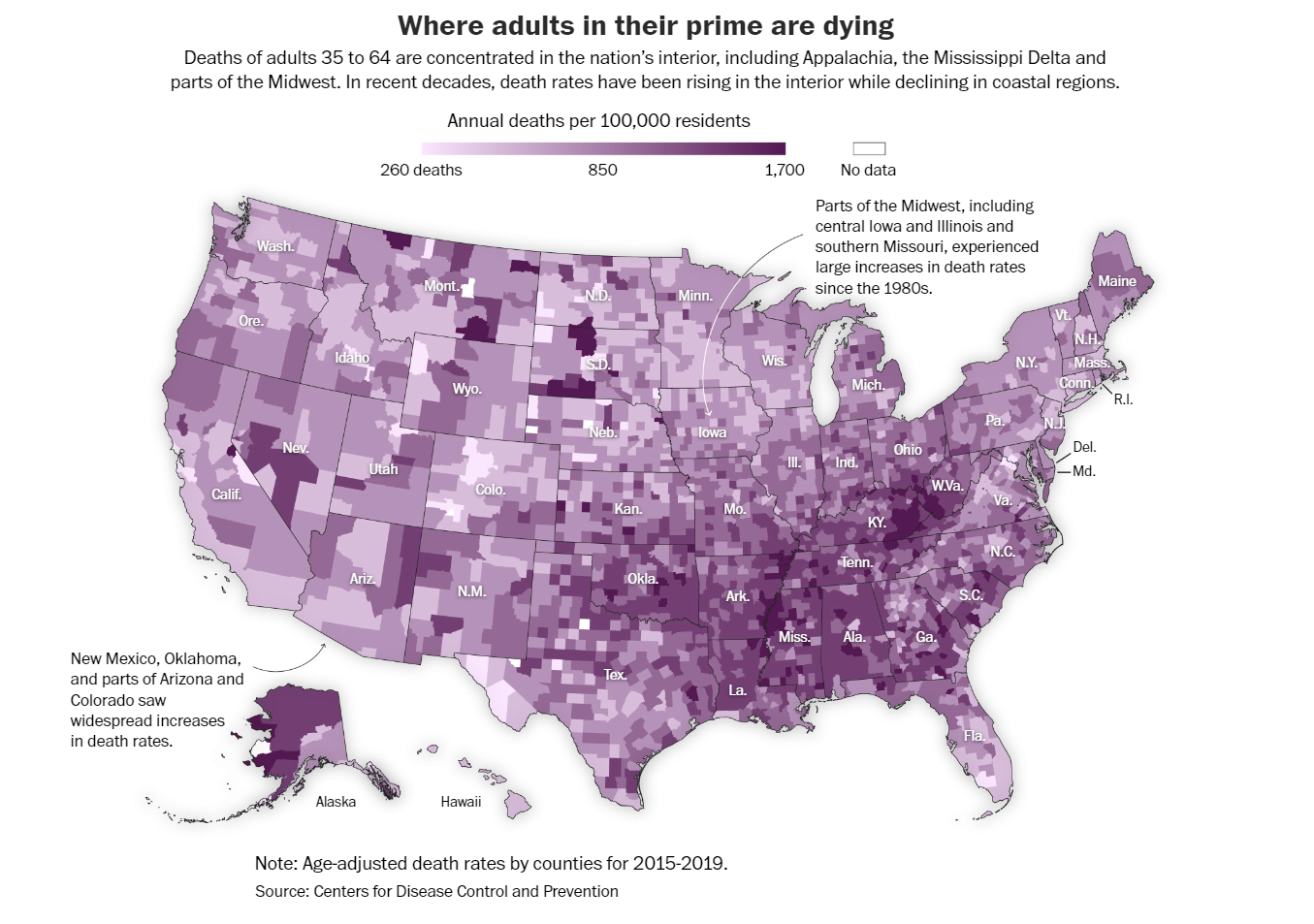
Figure 1: Centers for Disease Control and Prevention (CDC) in: Achenbach, Keating, McGinley, Johnson & Chikwendiu, Dying Early America’s Life Expectancy Crisis, Washington Post
Tom Morris, Associate Administrator for Rural Health Policy, Health Resources and Services Administration (HRSA), at the U.S. Department of Health and Human Services level-set the extent of health outcomes for Rural America, and how factors of place and race affect your quality of life. Our health as a nation is dwindling and declining, but the disparity of health and quality of life between metropolitan areas and rural areas in America is stark.
Morris shared data that amplified the importance of advancing Rural Health Equity. Rural women face higher maternal mortality rates. Rural residents have higher occurrences of mental and behavioral health diagnoses, which is compounded by the limited access to mental health care in these communities. On average, rural populations are less likely to have health insurance, and have fewer health insurance options than their urban counterparts. Emily Burleson, Project Manager of Advocacy & Research at PRT, shared on her panel that in 2019, there were 19 rural hospital closures, the highest count in a year to date. This shows the extent of diminishing access to care in regions where access was already lacking; rural residents are thereby forced to travel longer distances to seek care, posing other challenges to accessibility.
Morris also noted that risk factors such as obesity, smoking, exposure to environmental hazards, physical inactivity, occupational hazards, poverty, low-education, racial segregation and other indicators of early death are all increasing in prevalence in rural counties, but are decreasing in metro counties. Rural America drastically leads in individuals at higher risk of the five most preventable causes of death compared to metropolitan residents.
The trends in rural health are jarring. Health outcomes are even more bleak for rural regions of persistent poverty. A persistent poverty county is defined as a county that has 20% of the population below the poverty line for 30 years or more. This deep, systemic, and intentional condition has created pockets or regions where poverty has lingered for generations, compounding rural health, economic, and education disparities. The Regions PRT serves, including Appalachia, the Colonias, the Rural West, the Delta, the South, and Native lands, face even more bleak realities.
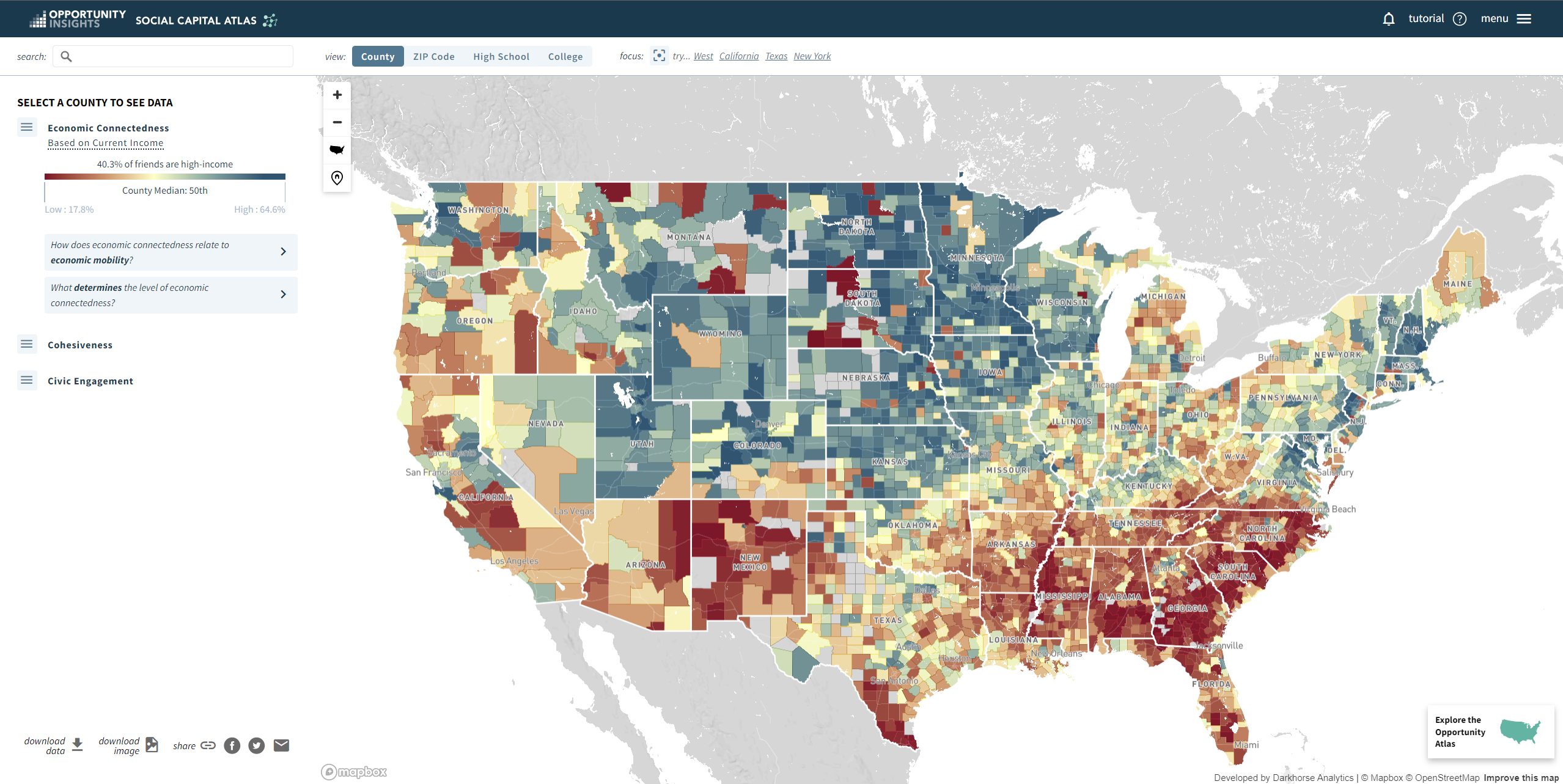
Figure 2: Social Capital Atlas, Opportunity Insights
These regions are persistently poor by design. They are results of intentional systemic racism, disinvestment, and marginalization. If you overlay the map of Persistent Poverty Counties, you will have the general shape for most other maps that show “poorer outcomes” across the country in a variety of topics (see figures 1, 2 and 3). It also mirrors maps of America’s history of enslavement, gentrification, and extraction of resources. These rural Persistent Poverty Counties face the same disparities as rural America overall, but at an exponential level.
PRT investigated the extent of the gaps for these persistently poor regions. The consequences of our history manifest in persistently poor regions today. We see it in inadequate community infrastructure, chronic disinvestment, high unemployment rates, banking and food deserts, lower than average access to safe drinking water, and more. 81% of Persistent Poverty Counties are in the bottom quartile of health outcomes across all counties in the country. In 42% of the 395 Persistent Poverty Counties, there were instances of health-related drinking violations, compared to the national average of around 37%. Of the 100 counties experiencing the highest occurrences of low birthweight babies and premature death, both of which are indicators of social and economic well-being in a child’s quality of life and life expectancy, 70 are counties of persistent poverty.
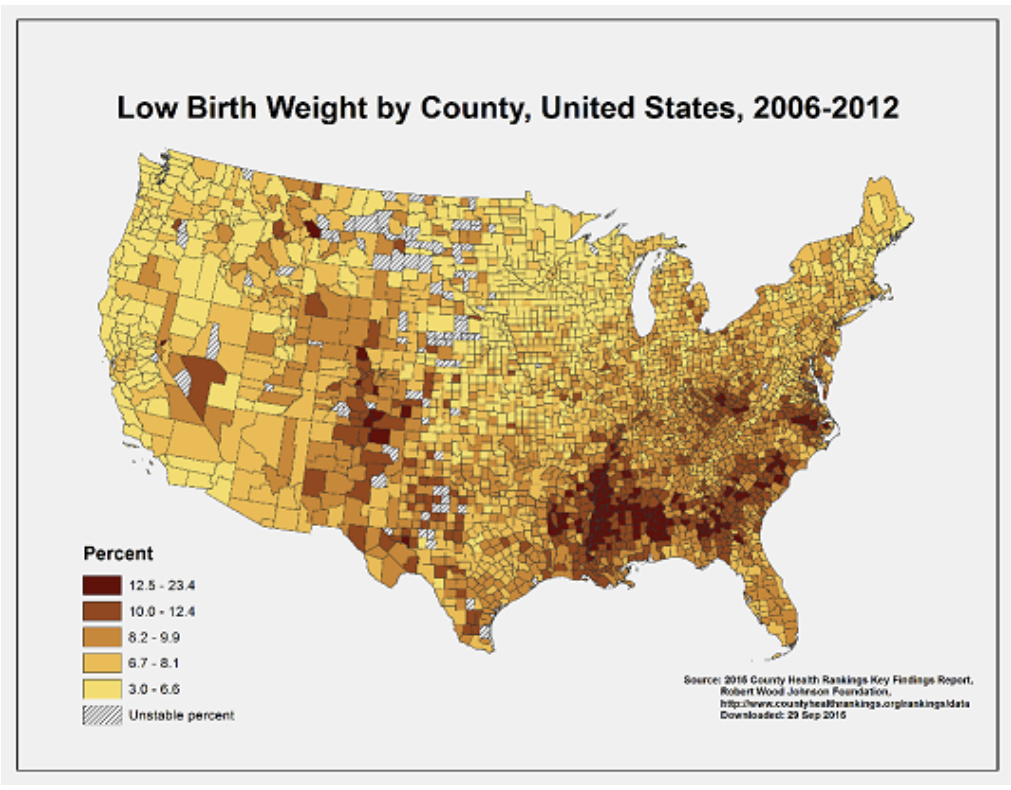
Figure 3: Low Birth Weight by County, United States, 2006-2012. Center for Disease Control and Prevention (CDC).
With the melancholy tone of the health outcomes for rural America, and the even worse health outcomes for persistently poor rural America, it is important to include that there are remedies that exist. PRT acknowledges that the various sectors we work across (housing, community facilities/infrastructure, business development, technical assistance, and more) all impact the physical and mental health of our rural neighbors. We work collaboratively across regions and sectors with trust and respect to generate holistic investment and community-led approaches to advance the rural health equity of communities.
The conversation of Advancing Rural Health Equity was held at a critical time, as our well-invested healthcare systems emphasizes symptom management and treatment, but general community wellness needs to come first. This event held panels discussing several angles to overcome racial and spatial inequities in health. The panels discussed broader barriers and solutions to financing health projects in rural and Native persistently impoverished areas, examples of successful health models in rural areas, and how to evaluate health projects in rural areas with evidence.
The last panel in particular teed up the noteworthy release of the newest rural health resource for practitioners and local community development leaders: a Guidebook on Leveraging Partnerships and Data to Improve Rural Health & Well-Being. The Guidebook is authored by Corianne Scally and her team at the Urban Institute, who co-hosted the event. The Guidebook includes a myriad of topics ranging from establishing partnerships, how to measure progress and evaluation of models in rural communities, and publicly available data for leveraging rural health funding, investment, and measuring project outcomes. The Guidebook is a wonderful tool for anyone who is looking to start understanding what health data exists, and some starting points on how to address health within a rural community.
The Partners for Rural Transformation call for other organizations to reflect on their impact on physical and mental health to their constituents and consider what CDFIs and other strategic partners with a shared mission of developing communities they should be reaching out to. If the Partners for Rural Transformation can help identify these connections or help establish them, or if you think we should be in contact with you and your organization, please reach out to prt@pfrt.org.
Read our colleague Urban Institute’s write-up here: https://www.urban.org/urban-wire/addressing-rural-health-disparities-requires-trust-data-and-focus-equity
